Research
Background
Within the estimated 2 million fungal species on earth, about 600 cause diseases in humans, and the most important are Candida, Aspergillus, Mucorales, and Cryptococcus. Fungal infections are increasing and are associated with excessive morbidity and mortality. Over 300 million people are acutely or chronically infected, leading to death, long term illness, and reduced work capacity. The reasons for emergence are likely multifactorial, eg the advent of medical progress, the successful application of immunosuppression in transplanted patients, and the use of immunomodulatory agents for treating various diseases from cancer to rheumatoid arthritis. Reducing the incidence relies on rapid and specific diagnostics, effective antifungal drugs, novel immunotherapeutic strategies, and adherence to infection control and sterility practices.
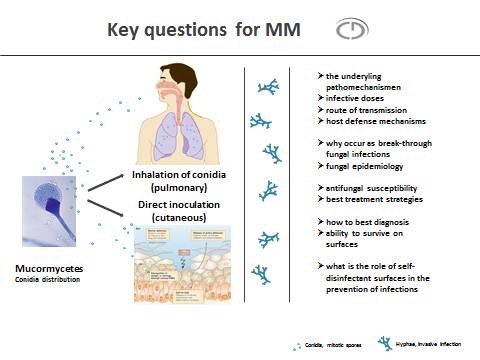 |
In conclusion, mucormycetes belong to emerging fungal pathogens and infections continue to rise, early diagnosis is difficult to obtain, treatment options are limited and outcome is very poor. Self-disinfecting surfaces and their potential in reducing nosocomial infections need to be evaluated in detail. The timing and need for CD-Fungus is spot on as currently the mycology field acknowledges that the traditional approaches to diagnose, treat and prevent MM have not lead to much progress. The prevention and control of health-care-associated and nosocomial infections has global significance. The World Health Organization announced the optimization of patient care and safety as inevitable highest priority for the 21st century.
Goals
CD-Fungus deals with the following three main research questions: How to best find, treat and prevent MM?
Tackling these key questions needs 1) recognizing MM as such 2) identification of the source and type of infection 3) identification of the pathogen 4) understanding the underlying pathomechanisms 5) initiation of early targeted treatment and 5) providing a clean and safe hospital environment.
CD-Fungus attempts to unravel scientific questions raised by implementing 3 modules which will ultimately advance our understanding of fungal pathology, improve diagnosis and treatment of MM and enhance patients’ outcome and safety in terms of prevention of nosocomial and hospital-associated infections.
Module 1. Pathophysiology of MM: from bench to bedside
 to unravel specific mechanisms underlying host and pathogen factors involved in the onset of MM,
to unravel specific mechanisms underlying host and pathogen factors involved in the onset of MM,
 to identify novel therapeutic strategies for the management of MM and to improve patients’ outcome.
to identify novel therapeutic strategies for the management of MM and to improve patients’ outcome.
Module 2. Improving fungal diagnosis
 to improve an existing molecular based diagnostic assay by expanding the fungal panel to be detected,
to improve an existing molecular based diagnostic assay by expanding the fungal panel to be detected,
 to improve an existing molecular based diagnostic assay by incorporating fungal resistance markers.
to improve an existing molecular based diagnostic assay by incorporating fungal resistance markers.
Module 3. The germ free hospital? Prevention of infections via antimicrobial EAS-technology
 to define the potency, efficacy, and long-term effectiveness of EAS-products,
to define the potency, efficacy, and long-term effectiveness of EAS-products,
 to estimate the impact of EAS on infections in experimental in vivo models,
to estimate the impact of EAS on infections in experimental in vivo models,
 to identify the anti-bacterial power of EAS in real-life at IMU.
to identify the anti-bacterial power of EAS in real-life at IMU.
 |
Christian Doppler Labor für invasive Pilzinfektionen
Kontakt:
CD Labor für invasive Pilzinfektionen
Schöpfstr. 41/2. Stock
A-6020 Innsbruck
Tel: +43 (0)512 9003-70703
Labor
Tel: +43 (0)512 9003-70721
Fax: +43 (0)512 9003-73700
E-Mail:
hygiene-bakteriologie@i-med.ac.at
Kontakt:
CD Labor für invasive Pilzinfektionen
Schöpfstr. 41/2. Stock
A-6020 Innsbruck
Tel: +43 (0)512 9003-70703
Labor
Tel: +43 (0)512 9003-70721
Fax: +43 (0)512 9003-73700
E-Mail:
hygiene-bakteriologie@i-med.ac.at




